
taking Blood Pressure correctly-
it's no
OFF-THE-CUFF
matter
You may take blood pressure readings every day- but just how accurate are your findings? Make sure you meet American Heart Association standards for this key assessment procedure by reviewing the guidelines here.
Breathless, Patty Smith arrives for her clinic visit a few minutes late. As you prepare to take her blood pressure, you learn that she's 39, single, and the mother of three preteen children.
Her blood pressure by arm cuff is 140/94 mm Hg- not surprising, you think, considering her obesity and her stressful life. You report your findings to the doctor, who schedules her for a follow-up visit and possible therapy for high blood pressure.
But is this really such an open-and-shut case? Or could the reading be falsely high because you used a normal-size adult cuff instead of one designed for larger persons? Perhaps Patty's blood pressure was temporarily high because she was harried and never stopped chattering about her trouble finding a sitter and a parking space.
Though the procedure seems simple, taking a blood pressure reading with a cuff is fraught with potential errors that can stand between you and a valid assessment of your patient's condition. These errors could leave a hypertensive patient untreated while a patient with normal blood pressure ends up on an expensive drug regimen he doesn't need. Either way, the patient loses.
What's more, keep in mind that a single measurement may not represent your patient's true blood pressure. The American Heart Association recommends this procedure: Take your patient's blood pressure twice while he's standing, then record the average of the two; next, take it twice while he's sitting and record the average of those two. Document which pressure was taken with the patient standing and which with him sitting. Use the sitting measurement as your final reading- the standing measurement is a reference point only.
Initially, take the blood pressure in each arm and document any difference in the reading. After that, use the arm that gave the higher reading.
Of course, measuring and assessing blood pressure is easy-provided you know the three possible sources of error: the equipment, the patient and the operator (you). Let's look at each one.
The equipment...
Errors can arise from uncalibrated or damaged equipment or from using the wrong equipment. (See Check for Problems before They Start.) Mercury manometers, for example, can yield inaccurate readings if the air vent at the top of the column is clogged or the mercury has oxidized. You may not spot these problems by looking at the manometer, but suspect them if the mercury column responds sluggishly. To prevent these problems, find out whether your institution has a written policy for regular assessment and maintenance of mercury manometers - and make sure to follow it.
With aneroid manometers, check before each use that the needle is on zero at baseline. If it isn't, recalibrate it to a mercury manometer using a Y connector attached to the tubing on both manometers. Compare pressures at several points along the scale. As with mercury mamometers, be sure this equipment is monitored and maintained regularly.
Incorrect cuff size is a major source of equipment-related errors. A cuff that's too small will produce a falsely high reading; one that's too large, a falsely low reading.
Using the wrong-size cuff is a common problem with obese patients. Taken with a regular cuff, their systolic and diastolic pressures will be falsely elevated. A similar potential for error exists for patients with extremely thin arms- for them, a regular-size cuff may be too big, leading to falsely low blood pressure readings.
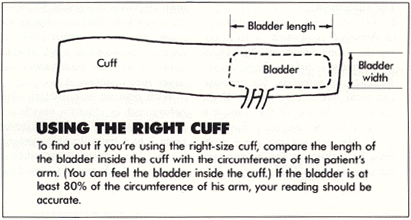
To check for proper cuff size, the American Heart Association recommends comparing the cuff with your patient's arm. The length of the bladder should be at least 80% of the arm's circumference. (See Using the Right Cuff.)
The stethoscope you use for auscultation should have a shallow bell with a large diameter. This lets you auscultate low-frequency sounds. (See What You're Measuring Isn't What You're hearing.)
Most nurses use the diaphragm of the stethoscope, but you should use the bell to auscultate indirect arterial blood pressures. Don't put too much pressure on the bell; you may occlude arterial flow and dampen out the low frequencies.
...the patient...
As you know, using too small a cuff to measure an obese person's blood pressure can cause a falsely elevated reading. You can also get a falsely high reading with a patient who has a peripheral edema-even if you use the right equipment. Like obesity, peripheral edema can diminish sound transmission, so avoid using edematous limbs to take blood pressure when possible.
Talking can also produce a falsely high measurement, as can pain, anxiety, or discomfort. Conversely, peripheral vasoconstriction, brought on by cold temperatures or vasopressors, decreases blood flow and can cause a falsely low reading.
Failing to support the patient's arm, which causes isometric muscle contraction, can also lead to false measurements. So be sure the patient's arm is supported and positioned at the level of his heart. Otherwise, hydrostatic and gravitational forces within the blood vessel will produce a false reading: If his arm is above heart level, you'll get a low reading; if it's below heart level, you'll get a high one.
In short, the more rested and relaxed your patient is while you're taking a reading, the more reliable your measurement will be.
...and you
The last major source of blood pressure error is the person taking the measurement. And in most instances, the problem is incorrect technique. (See 12 Steps to Taking Accurate Measurements.)
To ensure an accurate reading, position a mercury manometer with the meniscus at eye level and an aneroid manometer in your direct line of sight. To hear soft sounds that you might otherwise miss, deflate the cuff slowly.
Taking a patient's blood pressure correctly requires keeping your eye not just on the manometer but on the rest of the equipment, the patient,
and yourself as well. If you do, your efforts will translate into more effective practice for you and better care for
your patient.
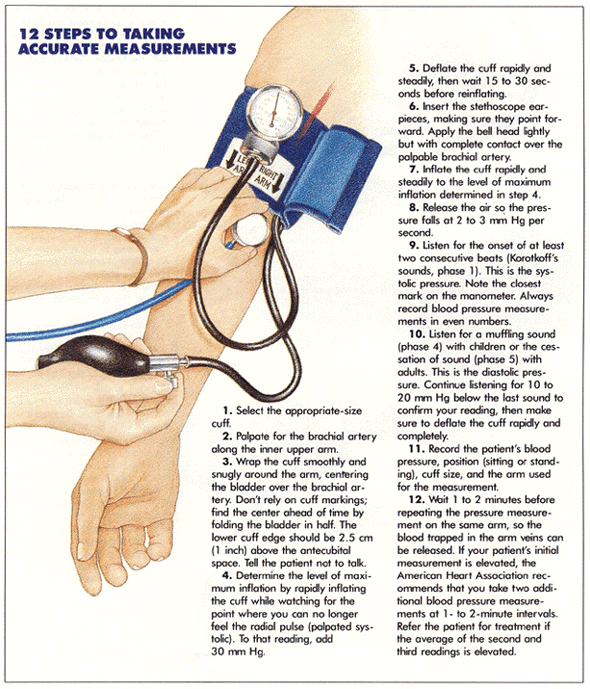
When you take a patient's blood pressure, you're measuring the pressure in the cuff- only indirectly are you measuring the pressure in the blood vessel. Here's why.
The mercury or aneroid manometer is attached to the cuff's bladder. When the pressure in that bladder exceeds their pressure in your patient's brachial artery, the artery is compressed and distal blood flow diminishes, then stops.
As you release the air in the cuff, the bladder deflates and cuff pressure falls. Then pressure in the cuff reaches the pressure generated by the heart during contraction, blood begins to flow through the artery again.
This flow produces Korotkoff's sounds: sharp topping or knocking sounds at each contraction. The cause of these sounds is still debated, but they may be caused by blood jetting through the partly occluded vessel. The jetting causes turbulence in the open vessel beyond the cuff.
According to the American Heart Association, Korotkoff's sounds occur in five phases.
Phase 1: faint, clear, tapping sounds. This is the systolic pressure.
Phase 2: murmurs or swishing sounds
Phase 3: crisper, more intense sounds
Phase 4: distinct, abrupt muffle of sound. In children, this is the diastolic pressure; in adults, it reveals hyperkintetic state (increased movement in blood vessels from disease or strenuous exercise) if it remains throughout deflation.
Phase 5: no longer any sound. This is diastolic pressure in adults.
Korotkoff's sounds have a frequency that's too low for the unaided human ear. Though you might estimate systolic pressure by
palpating the return of the pulse in the brachial artery, you can't detect diastolic pressure without a stethoscope's amplification.
CHECK FOR PROBLEMS BEFORE THEY START
Stethoscope
Cuff
Aneroid Manometer
Patient
A reprint from the November issue of Nursing94 by Springhouse Corporation, Springhouse, PA 19477.
A member of the Reed Elsevier plc group.
SELECTED REFERENCES
Byra-Cook, C., et al.: "Direct and Indirect Blood Pressure in Critical Care Patients," Nursing Research. 39(5):285-288, September/October 1990.
Henneman, E., and Henneman, P.: "Intricacies of Blood Pressure Measurment: Reexamining the Rituals," Heart & Lung. 18(3):263-273, May 1989.
Hill, M., and Grim, C.: "How to Take a Precise Blood Pressure," American Journal of Nursing. 91(2):38-42, February 1991.
The views expressed in this article are those of the authors and do not reflect the official policy or
position of the Department of the Army, the Department of Defense, or the United Staes Government.
Steele Supply Company and its affiliates are not responsible for typos in this reprint.
Steele Supply Company is not responsible for the accuracy of the information contained herein.
Stethoscope Information
Blood Pressure Information